Date:2026-03-04 10:00:50
A team at Yale School of Medicine has published a study detailing how its use of 3D surgical planning and 3D printing of patient-specific instrumentation is improving results in complex pediatric orthopedic surgeries.
David Frumberg, MD, Associate Professor of Orthopaedics and Rehabilitation at Yale School of Medicine, led the project, which has established a methodology for precision and reduced procedural complexity in the intricacies encountered when operating on children’s developing bone structures.
A team at Yale School of Medicine is using 3D surgical planning printing of patient-specific instrumentation to improve pediatric orthopedic surgical outcomes.
The team developed a workflow in which high-resolution CT scans are converted into digital 3D models, allowing surgeons to plan and rehearse procedures virtually before a patient enters the operating room. We recently reported on how a urological team at an Italian hospital is successfully using similar processes to reconstruct tumor-affected kidneys.
“Digital modeling allows us to see the hidden complexities of a child’s anatomy,” stated Frumberg. “We can then determine the best way to perform surgery on a computer multiple times before the patient even enters the operating room.”
Once a virtual surgical plan is finalized, engineers produce patient-specific instrumentation using medical-grade 3D printers. The custom guides are designed to fit a specific patient’s bone and direct the surgeon on where to cut and where to place screws, reducing reliance on freehand technique.
The research – published in Orthopedic Clinics – reported that in some cases, operative time was cut in half, intra-operative X-ray use declined, and limb alignment outcomes improved.
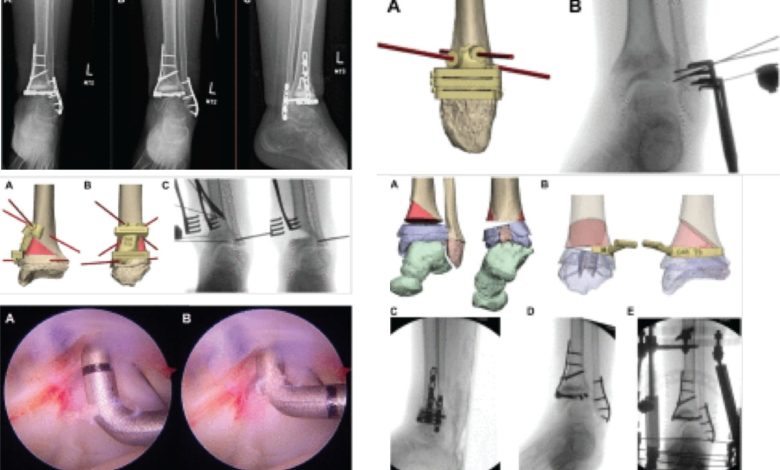
As a case study, the paper documented a 13-year-old patient with a severe lower tibia deformity caused by a rare medical condition. Standard surgical options would have required fusing the ankle joint, a procedure that would have significantly limited the patient’s long-term mobility.
“Instead, we used 3D planning to create a joint-preserving strategy,” Frumberg explained. “By using 3D-printed guides, we were able to reshape the inside of the ankle joint and restore its natural alignment. As a result, the young patient regained mobility and returned to the activities he loved.”
The technology appears set to become a standardized tool for a wider range of orthopedic procedures as it becomes more accessible.
“The goal of using 3D surgical planning is simple: improving the lives of children through better technology,” added Frumberg. “It means a surgery is less about ‘one size fits all’ and more about a custom-tailored path to an individual’s recovery.”